CASE REPORT 6
This case features an ankle
ulcer that had developed
significant slough and
required frequent
dressing change.
The patient in this case was a
96-year-old woman who lived in a
care home. Her nutritional status
was poor and she also had diabetes,
but was a non-smoker. Due to the
pressure ulcer that had developed on
her ankle she had been prescribed
systemic antibiotics by her GP and
was referred to tissue viability. The
wound had been present for four
weeks and was being treated daily
by the staff at the nursing home.
The ulcer itself measured 2x1cm
and the wound bed exhibited thin,
yellow slough, although there were
no signs of infection (
Figure 1
). The
periwound skin was healthy.
Wound progression
At presentation the dressing was
being changed daily and this was
reduced to every three days during
the evaluation period. Actilite
Protect (10x10cm) was used without
a secondary dressing. The clinician
felt that the size was possibly too
big for the wound, but still rated
the dressing as very easy to use and
remove, and easy to apply.
The wound’s dimensions did not
change throughout the evaluation
but by the end of week one the
slough was lifting and by week two
there was no slough at all, with the
wound bed having developed 100%
granulation tissue (
Figure 2
). The
patient’s pain was rated as ‘3’ on
a 1–10 scale, where ‘1’ indicated a
‘complete lack of pain’— this rating
reduced to ‘2’ after one week of
treatment with Actilite Protect.
The dressing was atraumatic to
the wound bed and the periwound
skin and conformed very well to
the wound. There was no pain
during wear and removal, and no
analgesics were required.
The dressing remained intact
on removal and it stayed in place
longer than expected, although it
did roll at the edges. The care home
staff needed to be persuaded to
change the dressing less frequently
(every three days), as they had been
used to daily changes.
The clinician felt that the Manuka
honey element of the dressing
helped to treat infection and
slough, and that the dressing made
a positive contribution to healing.
Overall, the clinician was very happy
with the dressing.
When the patient was asked
about the dressing she said that she
found it comfortable and pain-free —
overall she declared herself satisfied
with the treatment she had received.
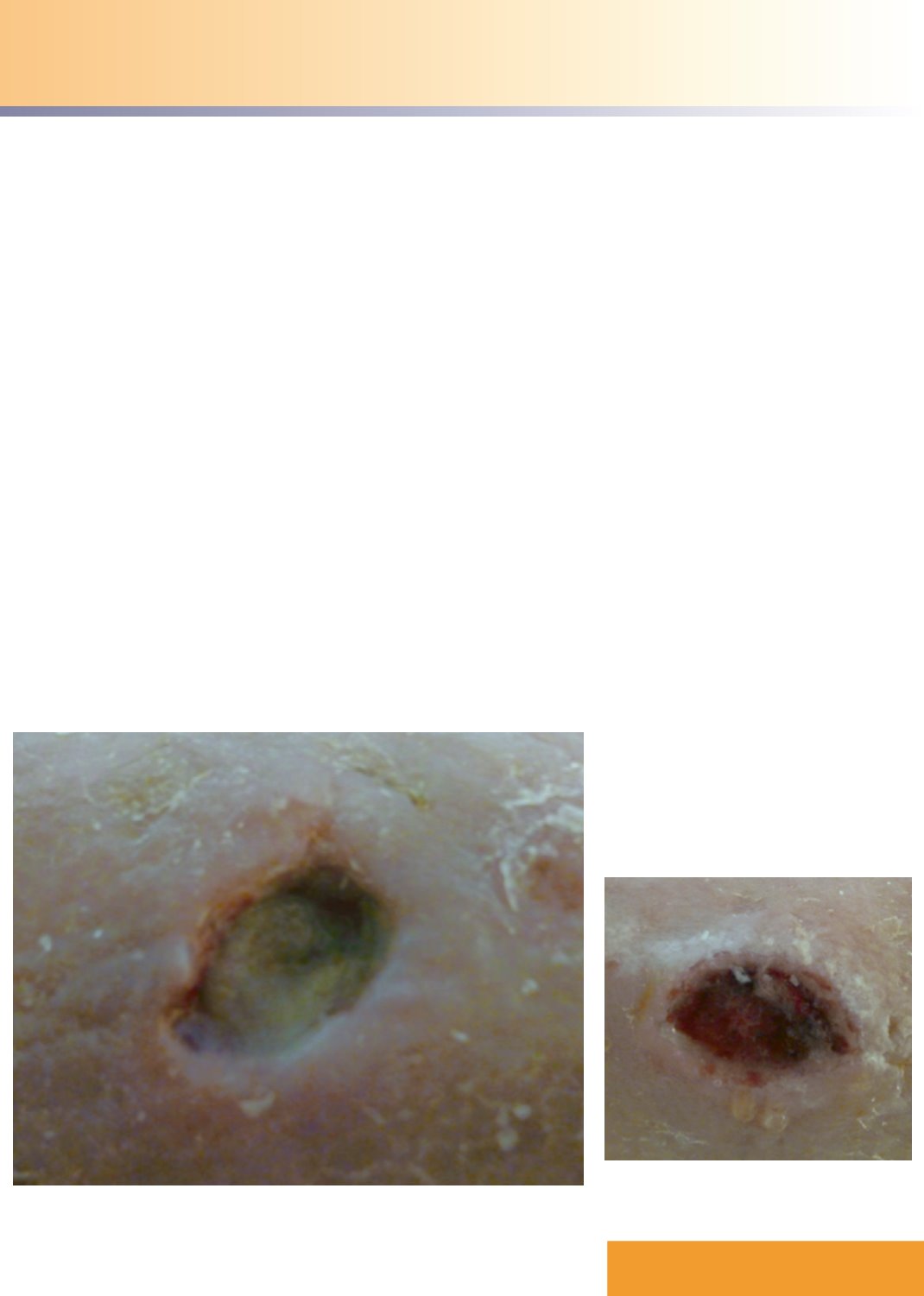
Figure 1.
The ulcer at presentation showing slough in the wound bed.
Figure 2.
At week two, the wound demonstrated
100% granulating tissue.
JCN supplement
2015,Vol 29, No 4
9








